Date: 06.11.19
Duration: 1300-1700
Individual with whom I worked with: Mick Smirthwaite
Before my placement:
Aims from today’s placement:
- To accept that I am in a safe learning environment and it is okay if I don’t know everything
- To observe assessment and treatment of clients who visit the clinic
- To listen to each client and gain a clinical impression of their injury or the source of their muscle tightness
- To observe Mick’s massage techniques and ask questions to establish the rationale for their application
- To establish the stage of healing and understand why certain treatments and modalities are used
- To be given the opportunity to use palpation skills and massage techniques
- To take photos of injuries and treatments used with the client’s permission
I need to be mindful of:
- Client confidentiality
- Health & Safety in the clinic environment
- My own personal presentation
- Hygiene in the clinic environment
Do I need to be aware of particular theories:
- I need to be aware of the relevant anatomy for each case
- To try and remember the special tests to rule out or confirm my clinical impression of an injury from information obtained during the subjective assessment
- To understand the soft tissue techniques used and be able to apply them
- To be aware of physiology and the stages of tissue and bone healing.
The ‘What Ifs’:
I have thought about the ‘What Ifs’ but they haven’t changed from the ‘What Ifs’ that I included in my reflection last week. I am less nervous than last week but being in the clinic environment, as a novice, is still challenging for me.
During my placement:
I felt more relaxed during the afternoon clinic. I knew that one of the appointments was going to be a follow-up appointment from last week.
As a novice I am expecting to see and experience new things. I did not feel uncomfortable or worried as sports therapy treatment isn’t always straight forward. There are so many different variables involved in establishing the mechanism of injury and the source of pain. It is like a puzzle and you have to find the right pieces in order to get the full picture.
After my placement:
When I arrived at the clinic, Mick was with a client. We started a little later as the treatment went over the hour. After the client had left, Mick did not have an appointment for the following hour, so we talked about the clients that he had scheduled for the afternoon.
I asked Mick about his recovery from his Quadratus Lumborum strain that he had acquired on Sunday 27th October. I had read up about the muscle, its specific location in the lumbar region, the muscle’s origin and insertion and its specific movement and role in the body. The muscle laterally tilts the pelvis, laterally flexes the vertebral column to the same side, assists in extending the vertebral column and bilaterally fixes the last rib during forced inhalation and forced exhalation (Biel & Dorn, 2014). Mick had believed that the mechanism of injury was hoovering, however he had mentioned that he had run earlier in the day and that it had “nearly killed him”. I believe that the forced inhalation and exhalation during his run was actually the mechanism of injury and that hoovering his house later aggravated it further. He agreed that this was indeed possible and said that it was feeling much better.
During our conversation I reflected upon last week’s clinic and said how much I had enjoyed it. I had learned a lot from observing Mick. It had motivated me and inspired me and I went home afterwards feeling extremely positive.
The first client, Mr D, had been a client of Mick’s for 6 years. He made an appointment today because he needed a sports massage after a challenging weight training session. He had a brief discussion with Mick regarding his general health, the activities he had been engaged in and the particular areas that he wanted Mick to focus on. His shoulders were particularly tender. He also quite strongly stated that he did not want his legs massaged as they were very sore. Mick asked the client to lay on the massage bed in the prone position. Mick began palpating the Quadratus Lumborum and Erector Spinae muscles on the left and right side of the body. He also palpated the Gluteal muscles. There was tension in the Gluteus Medius. Mick applied effleurage, both superficial and deep and slow tissue release (STR) with the hip adducted and the knee flexed. The same techniques were applied on the left side. Mick allowed me to apply effleurage to the lower back. Mr D was a large man and it was quite difficult to massage the muscle tissue deeply. I may need to think about massaging larger clients from a different angle, or from the opposite side of the couch to be able to get deeper into the muscle tissue. The muscles in the lower back were quite tight and Mick applied NMT and cross friction techniques as well as deep effleurage to release the tension and improve ROM. I quite enjoying observing Mick while he works and can identify the techniques being applied.
Mick moved onto the upper body and started palpating quite deeply into Deltoid and rotator cuff muscles on both sides of the body. He palpated deeply beneath the Deltoid and placed my thumb into the same spot (both left and right side of the body). He asked me what my impression was of the muscles. The rotator cuff muscle on the left side of the body was much tighter. It felt harder. I thought it was Teres Minor but it was actually the Infraspinatus. Of course it was! Why did I not remember that! Mick started massaging the Supraspinatus and Deltoid and progressed onto the Infraspinatus. He applied deeper massage and the client chose to reveal that he had experienced tingling down the left arm and that it sometimes felt numb when he was sat at a desk. Mick palpated quite deeply into the deltoid and the Infraspinatus. He also abducted the arm. He repeated this process a number of times applying NMT. Originally during observation I thought that the nerve being impinged was the Ulnar nerve, however after looking at my anatomy book and a paper regarding peripheral nerve impingement (Neal & Fields, 2010), I now believe that the nerve being impinged was the Axillary nerve.
The rest of the treatment involved massage of the hamstrings and calves, while the patient was still in the prone position. Deep massage was applied to the hamstrings when they were in slight knee flexion. The client turned onto his back and Mick applied the standard massage techniques to the Pectoral Major in the chest, the Quadriceps muscles and the extensors in the lower limbs.
The second client of the afternoon was a follow-up appointment with the gentlemen (the roofer, Mr M) came to Mick for treatment of a torn hamstring. The client said that the injury was much improved and that he could now walk up and downstairs. The injury was not as a painful as the previous week and it was feeling much better particularly in the last 3 days.
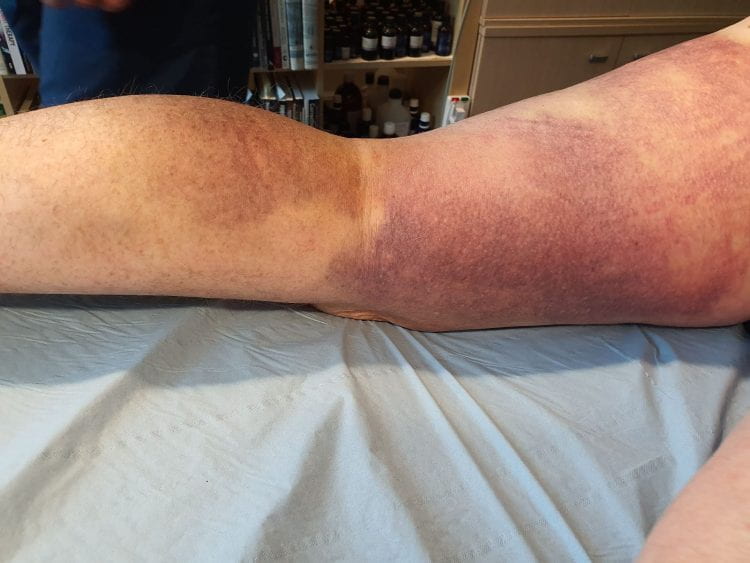
Upon examination we could see that the bruising had come out a lot more. We asked the client for his permission to take a photo for my Edublogs site and he confirmed that he was quite happy for me to do so. Photos are included below:
Figure 1
It was easier to see the origin of the trauma (area of most haemarthroses) in the middle of the back of the thigh and medial side of the leg. Mick allowed me to palpate the area and I noticed straight away that the muscle tissue was not has hard or as tense as last week.
Mick applied superficial effleurage and STR. He also massaged across the fibres and applied cross friction massage. Not the technique that we were taught in year 1, but a technique that I haven’t seen before. He decided to apply a fan taping, usually referred to as an Oedema Taping (with Kinesiology tape [KT]) to help draw the blood away from the muscle tissue. KT lifts the layers of skin and increases the interstitial space. This improves blood and lymphatic flow to reduce pain and alleviate swelling. I did not realise that it could be used to help draw blood out of the muscle tissue, but it makes perfect sense. The increased interstitial space and improved blood and lymphatic flow allows waste products to be removed from the injured area and allows oxygen and nutrients to flow to the damaged area, enhancing the healing process. I have used this technique before in Year 1 to reduce the swelling of a case of Housemaids knee. It was my case study for my soft tissue module. I understood immediately why it was being applied. I observed Mick prepare the tape and apply it to the back of client’s left thigh. I have included a photo of the taping below:
Figure 2
How I felt through-out my placement today:
I wasn’t so anxious today and I was looking forward to observing new cases and learning from them. I was very pleased and felt completely involved throughout the afternoon clinic.
Evaluate today’s placement activity:
I didn’t feel that anything went badly and had no negative thoughts or feelings at all. I enjoyed observing the assessment and treatment of both clients. Both very different cases but equally interesting.
A deeper, analytical and critical approach to today’s experiences:
Today’s experience was very positive. I didn’t feel that anything went badly. I mostly observed the assessment process and the treatments applied. I asked questions to gain answers that would help me gain a better understanding of why a particular massage technique was being applied or why Mick chose the treatment that he used. I will research the use of K-tape to clear bruising and blood in muscle tissues and to understand how it enhances the healing of the muscle tissue. I will also revisit the physiology of the tissue healing process.
Draw conclusions – what have I learned from today’s activities and my reflections:
Today I saw a cross friction massage technique that I haven’t seen before and will research it via YouTube and other soft tissue massage text books.
I hadn’t thought of using K-tape to remove blood in the muscle tissue. I have only ever used K-tape to help reduce inflammation and pain.
Action plan – how will I apply what I have learned from today’s activities & my future professional and personal development:
I will continue to practise my palpation skills – specifically rotator cuff muscles.
Research cross friction massage techniques via soft tissue massage text books and videos online.
Research the use of K-tape to draw blood out of muscle tissue.
Continue to revise my anatomy knowledge to keep it fresh.
Have any questions arisen from today’s placement that I need to discuss with my Placement Tutor or University Placement Tutor:
I don’t have any questions about today’s placement experience. I usually ask questions during the observation to either confirm what I think is going on or to correct my assumptions, thoughts if they are incorrect.
Returning to my reflections:
I did some investigation into whether there was any current research into the beneficial effects of the use of K-tape on haematomas in muscle tissue after a tear. Currently there does not appear to be any research evidence that k-tape reduces bruises in muscle tissue. Only subjective and anecdotal evidence exists showing the dramatic effect of the application of k-tape on bruises (“Kinesiology tape research | RockTape,” 2018). There is evidence however regarding the effectiveness of K-tape together with soft tissue massage in reducing inflammation (Biaoszewski, Woÿniak, & Slawomir, 2009).
References:
Biaoszewski, D., Woÿniak, W., & Slawomir, Z. (2009). Clinical efficacy of Kinesiology Taping in Reducing Edema of the Lower Limbs in Patients Treated with the Ilizarov Method. Ortopediia Traumatologia Rehabilitacja, 11(6), 46–54.
Biel, A., & Dorn, R. (2014). Trail guide to the body : a hands-on guide to locating muscles, bones and more (5th editio). Boulder, CO, ISA: Books of Discovery.
Kinesiology tape research | RockTape. (2018). Retrieved May 31, 2020, from https://rocktape.com.au/kinesiology-tape-research/
Neal, S. L., & Fields, K. B. (2010). Peripheral nerve entrapment and injury in the upper extremity. American Family Physician, 81(2), 147–155.