Prehabilitation has been given the definition of “the process of enhancing functional capacity of the individual to enable them to withstand the stressor of inactivity” (Ditmyer et al. (2002), the preparation a patient before a stressful event. Prehabilitation is a pre-emptive, preventive method to exercise designed to maximise the chances of not getting injured. The theory was originally thought of in the 1980s for athletes as a preventable process in which to avoid atrophy of muscle in order to prevent future injuries (Spain et al. (1984). Additionally, prehabilitation can also be used in the time lead up to having a total knee replacement (Swank et al. (2011), and other injury procedures, such as in this case, an ACL rupture (Alkarmi et al. (2010).
The rehabilitation of injured populations undergoing anterior cruciate ligament (ACL) reconstruction requires symmetry in strength and sufficient proprioception abilities preceding any return to the preoperative level of which the patient played sport. This will be the factor which can delay the patients return to play. On the subject of prehabilitation, involving an ACL injury, there appears to be little literature. This article discusses the anatomy, biomechanics, uses of strength training and any other existing knowledge of “prehabilitation” in those with an ACL injury.
This injury is regarded as joint instability that primes to pain, poor function and common injury reoccurrence, and also has a higher risk of osteoarthritis. Somewhat little research has been looked into the effects preoperative strengthening of the Anterior Crucial Ligament (ACL) can have on the injured patient.
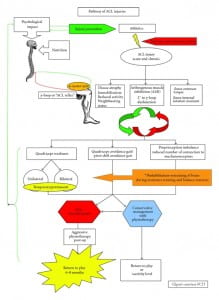
Figure 1. The pathway of the ACL-injured patient and the role of prehabilitation
Biomechanics in ACL-Deficient Knees
The symptoms of knee instability with an ACL rupture come about all through the weight receiving of the limb that is injured in the early stance phase of the gait cycle (Shaarani et al. (2012). During the phase of the cycle, the limb takes complete support of the body and diminishes shock through the use of knee flexion, this is restricted by eccentric contraction from the quadriceps. This small modification in movement pattern consequences from the indecision to fully engage the quadriceps muscles when the knee is at the end range on the point of full knee extension. However, these altered kinetic movements persist following ACL reconstruction (Bulgheroni et al. (1997); Davy et al. (1987), suggestive of that instability being not the singular source of the gait adaptation.
Strength Training
A 5-week prehabilitation plan that consist of progressive muscle strengthening exercises has been proven to show a considerably improved knee function, quadriceps peak torque, and the total workings within patients with an ACL injury (Eitzen et al. (2010).
Keays et al. enlisted patients with prolonged ACL injuries in a pre-rehabilitation programme that would last the duration of 4–6-weeks, followed by a rehabilitation programme that ran a minimum of 4-months after surgery Keays et al. (2000]. Their performance in the side step, carioca, and shuttle run improved considerably. Research has assessed plyometric training, with the prevention of anterior cruciate ligament (ACL) injuries. Developing evidence point toward plyometric exercises and training may help prevent ACL injuries. (Tagesson et al. (2008), report the use of a plyometric program can increase neuromuscular control on three planes which will decrease stress on the ACL and transfer it to the muscles, tendons and bones. Thus, giving improved force dispersal meaning less torque to the knee. Following 6 weeks of exercise intervention, (Strocchi et al. (1992) reports the single-legged hop test results improved significantly. Quadriceps peak torque in the injured limb improved with similar gains in CSA compared with the baseline test group.
Plyometrics is similar to strength training; the resulting aim is to develop physical power. Plyometrics emphases on the speed element of power and will alter the functional changes into athletic ability developing more powerful concentric contractions (Harrison & Gaffney, 2001; Hennessy & Kilty, 2001). Rimmer & Sleivert (2000). The addition of an eccentric contraction prior to a concentric contraction has been found to increase the force, speed, and power output of the concentric contraction (Wilk et al., 1993). How you ask? Stretch shortening cycle (SSC).
The two mechanisms that contribute to the explosive concentric contraction are the muscle spindles and the elastic potential of the muscle by use of the stretch reflex (Figure 1) (Bosco et al., 1979, 1981, 1982). The stretch reflex is described by (Guyton and Hall 1995; Matthews 1990) to be the body’s involuntary response to an external stimulus that stretches the muscles.
During the use of plyometric exercises, muscle spindles are stimulated by a quick stretch. The muscle spindles are proprioceptive organs that are delicate to the rate and scale of a stretch, when a quick stretch is detected, muscular activity increases initiating a reflective muscle action. This strengthens the force that muscle then produces (Kilani et al., 1989). Functioning similar to a rubber band, when stretched, adds to the power of when it is released. However, if the concentric action is not closely followed by a stretch, the stretch reflex is cancelled.
 Figure 3. Here is a diagram of the stretch reflex. Once the stretch reflex is stimulated it sends input to the spinal cord via the nerve fibres. Once a connection with the alpha motor neurons occur, impulses are sent to the agonist fibres triggering a muscle action.
Figure 3. Here is a diagram of the stretch reflex. Once the stretch reflex is stimulated it sends input to the spinal cord via the nerve fibres. Once a connection with the alpha motor neurons occur, impulses are sent to the agonist fibres triggering a muscle action.
In everyday activity, due to the forces of gravity, compression and impact forces, from running and jumping activities, there will be an eccentric contraction shadowed by a concentric contraction. During any type of jumping activity, this quick stretching of the muscles on landing causes the spindles to be triggered and in so doing so add to the power output following SSC movements.
Plyometrics & Agility Training This video explains the use of preventative exercise techniques
References
Alkarmi, A. Thijssen, D. H. J. Albouaini, K. (2010). “Arterial prehabilitation: can exercise induce changes in artery size and function that decrease complications of catheterization?” Sports Medicine, vol. 40, no. 6, pp. 481–492, 2010
Bosco, C. Komi, P.V (1981) Potentiation of the mechanical behaviour of the human skeletal muscle through prestretching, Acta Physiological. Scand 111:135-140.
Bulgheroni, P. Bulgheroni, M. V. Andrini, L. Guffanti, P. and Giughello A. (1997), “Gait patterns after anterior cruciate ligament reconstruction,” Knee Surgery, Sports Traumatology, Arthroscopy, vol. 5, no. 1, pp. 14–21, 1997
Davy, D. T. and Audu, M. L. (1987). “A dynamic optimization technique for predicting muscle forces in the swing phase of gait,” Journal of Biomechanics, vol. 20, no. 2, pp. 187–201, 1987
Ditmyer, M. Topp, M. R. and Pifer, M. (2002). “Prehabilitation in preparation for orthopaedic surgery,” Orthopaedic Nursing, vol. 21, no. 5, pp. 43–52, 2002
Eitzen, I. Moksnes, H. Snyder-Mackler, L. and Risberg, M. A. (2010). “A progressive 5-week exercise therapy program leads to significant improvement in knee function early after anterior cruciate ligament injury,” Journal of Orthopaedic and Sports Physical Therapy, vol. 40, no. 11, pp. 705–721
Guyton, A.C. Hall, J.E. (1995) Textbook of Medical Physiology, 9th edition Philadelphia: Saunders.
Harrison, A.J. Gaffney, S. (2001). Motor development and gender effect on stretch shortening cycle performance, Department of Physical Education and Sports Science, University of Limerick, Limerick, Ireland
Hennessy, L. and Kilty, J. (2001) Relationship of the Stretch-Shortening Cycle to Sprint Performance in Trained Female Athletes. Journal of Strength and Conditioning Research, 15 (3), pp. 326-331.
Keays, S. L. Bullock-Saxton, J. and Keays, A. C. (2000)., “Strength and function before and after anterior cruciate ligament reconstruction,” Clinical Orthopaedics and Related Research, no. 373, pp. 174–183, 2000.
Kilani, H.A. Palmer, S.S. Adrian, M.J. Gapsis, J.J (1989) Block of the stretch reflex of vastus lateralis during vertical jump Human Movement Science 8:247-269.
Matthews, P.B.C. (1990) The knee jerk: Still an enigma? Journal of Physiological Pharmacal 68:347-354.
Rimmer, E, & Sleivert, G. (2000). Effects of a plyometrics intervention program on sprint performance. Journal of Strength and Conditioning Research 14, (3), 295-301.
Shaarani, S. R. O’Hare C, Quinn A, Moyna N, Moran R, O’Byrne JM (2012) Prehabilitation: The Void in the Management of Anterior Cruciate Ligament Injuries—A Clinical Review
Spain, J. (1985) “Prehabilitation,” Clinics in Sports Medicine, vol. 4, no. 3, pp. 575–585, 1985
Strocchi, R. de Pasquale, V. Gubellini P. et al. (1992). “The human anterior cruciate ligament: histological and ultrastructural observations,” Journal of Anatomy, vol. 180, no. 3, pp. 515–519, 1992.
Swank, A. M. Kachelman, J. B. Bibeau, W. (2011) “Prehabilitation before total knee arthroplasty increases strength and function in older adults with severe osteoarthritis,” ,” Journal of Strength and Conditioning Research, vol. 25, no. 2, pp. 318–325, 2011
Tagesson, S. (2008) Dynamic knee stability after anterior cruciate ligament injury: emphasis on rehabilitation, [Ph.D. thesis], Linköping University, Linköping, Sweden, 2008, Linköping University Medical Dissertations no. 1036.
Wilk, K.E. Voight, M.L. Keirns, M.A. Gambetta, V. Andrews, J.R. Dillman, C.J (1993) Stretch-shortening drills for the upper extremities. Theory and Clinical Application Journal of Orthopedix Sports Physiotheraphy 17: 225-239.
HAPProf’s channel. (6 Feb 2008). The Stretch Reflex. Available:https://www.youtube.com/watch?v=HfuhVWK8C0U . Last accessed 17th March 2016.
3D Anatomica. (2 Jan 2010). ACL Tear (Sports Injury) . Available: https://youtu.be/lpIOMuqXWrE. Last accessed: 17th March 2016.
Figure 1, Pathway of ACL Injury. Shaarani, S. R. O’Hare C, Quinn A, Moyna N, Moran R, O’Byrne JM (2012). Prehabilitation: The Void in the Management of Anterior Cruciate Ligament Injuries.
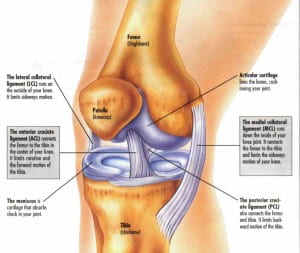
Figure 2, Knee Anatomy Diagram Ligaments. Available: http://healthfavo.com/knee-anatomy-diagram-2.html Accessed on: 17th March 2016.
Figure 3, Muscle Spindle Stretch Reflex. Available:http://www.lookfordiagnosis.com/mesh_info.php?term=Reflex%2C+Stretch&lang=1 Accessed on: 17th March 2016.